For years, treatment meant one bulky machine and a lot of frustration.
For a long time, the story around sleep apnea treatment felt stuck.You got diagnosed, you got handed a mask and a machine, and that was more or less the deal. For plenty of people, that setup still works and remains the frontline treatment. But it also became the reason a lot of patients dropped off, delayed care or never really stuck with therapy in the first place. What is changing now is not that the old machine has disappeared. It is that the market around sleep apnea is finally opening up.
That matters because sleep apnea is not a niche problem
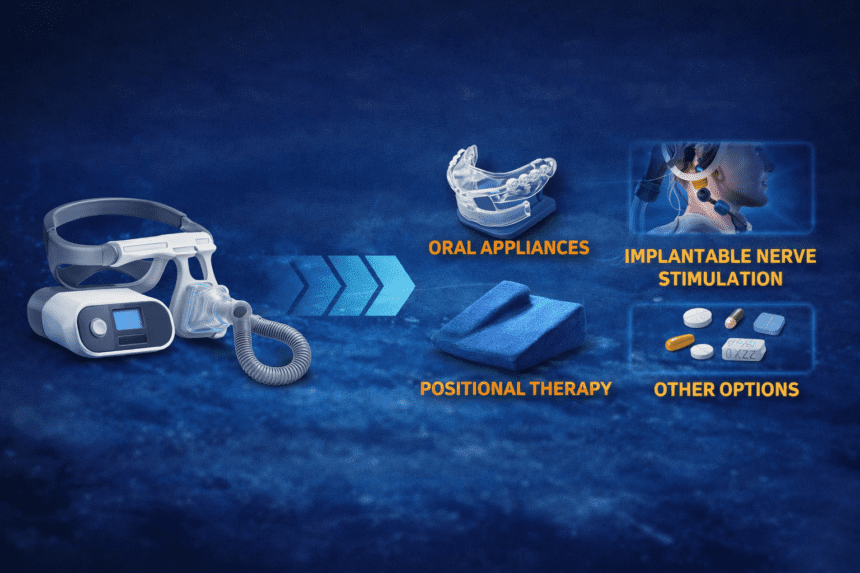
Obstructive sleep apnea treatment is aimed at keeping the airway open during sleep and reducing repeated breathing interruptions, and treatment options now range from positive airway pressure devices to oral appliances, surgery, nerve-stimulation implants, medications and lifestyle changes, depending on the patient and the cause. That wider menu is the real shift. The old one-size-fits-all model is giving way to something more tailored. The headline change is simple: treatment is becoming less binary, instead of the old choice between “use the mask” or “do nothing,” patients are increasingly being offered alternatives that sit across a spectrum. Some are less invasive, like oral appliances that help reposition the jaw during sleep. Others are much more high-tech, including implantable systems that stimulate the nerve controlling tongue movement to help keep the airway open. Recent reviews describe this as a shift toward personalised, multimodal management rather than a single default solution for everyone.
That is where the most interesting tech story sits
One of the biggest areas of momentum is nerve stimulation. These implanted systems are designed for adults with obstructive sleep apnea who cannot tolerate or have not responded to first-line treatment. The basic concept is to stimulate the hypoglossal nerve during sleep so the tongue moves forward and the airway stays more open. Coverage documents, clinical reviews and recent medical reporting all point to this category becoming a more established part of the treatment landscape rather than an experimental outlier and that category is still moving, Recent medical reporting said a new hypoglossal nerve stimulation technology had been approved, while other current reports describe fresh approvals for additional implanted systems for adults with moderate to severe obstructive sleep apnea who cannot tolerate first-line treatment. Even allowing for differences between markets and patient eligibility, the broader direction is clear: device makers are no longer building around a single dominant pathway. They are competing to offer more targeted options.
That does not mean the old machine is dead
Positive airway pressure therapy is still widely described as the most common and effective treatment for obstructive sleep apnea, especially as first-line care. The real change is that it no longer has the field to itself in the public imagination or in clinical pathways. For years, sleep apnea tech was largely defined by improving the same basic hardware. Now the category is being reshaped by alternatives designed around comfort, adherence and better fit for different types of patients, that is important because adherence is everything.
A treatment only works if people actually use it. That has always been the weak point in sleep apnea care. The expansion of oral appliances, positional therapy, implantable stimulation and other non-CPAP approaches reflects a bigger recognition inside sleep medicine: the best treatment on paper is not necessarily the best treatment for the patient if they cannot live with it night after night. Recent reviews explicitly frame the field around phenotype-guided and multimodal care, which is a more sophisticated way of saying patients need different solutions.
There is also a broader health tech angle here
Sleep medicine is starting to look more like the rest of consumer and medical technology, where categories fragment, user experience matters, and legacy hardware gets challenged by more flexible systems. That does not mean every new treatment will be right for every patient, and it definitely does not mean every gadget marketed around sleep deserves serious attention. But the treatment side of sleep apnea is clearly moving from a single device era into a platform era.
That is the real takeaway
The story is not that one old treatment has suddenly failed. It is that the market is finally admitting what patients have known for years: a lot of people need something different. The next phase of sleep apnea care looks less like a universal machine and more like a layered toolkit built around who the patient is, what they can tolerate and what actually keeps them breathing through the night.